Reconstructive Procedures: Head and Neck Reconstructive Surgery
Table of Contents
Head And Neck Reconstructive Surgery
What is head and neck reconstruction?
What parts of the head and neck can be reconstructed?
The head and neck are made up of complex anatomical structures responsible for vital functions such as breathing, eating, and speech. For example, the tongue has multiple intrinsic and extrinsic muscles as well as external lining, which needs to be reconstructed appropriately to enable swallowing and speaking.
Together with you and the resecting surgeon (if any), your plastic surgeon will assess the expected defect and discuss the appropriate options for reconstruction with you.
What can I expect from my procedure?
To achieve this, the reconstructive surgeon utilizes a combination of procedures including grafts, prosthetics, and tissue transfer (flaps) from the patient to replace missing structures with similar tissue, akin to transplantation within the individual. Flaps refer to tissue with their own blood supply taken from one part of your body that does not need it to replace missing tissue in an area which requires it. These flaps can be from around the area of the defect (local flaps), further away but keeping their blood supply intact (regional or pedicled flaps), or from distant sites where blood supply is re-established at the defect site (free flaps). The type of flap used will be dependent on location, size, and composition of the defect. Our board-certified plastic surgeon is very familiar with free flap reconstruction of the head and neck and will discuss the options for your reconstructive surgery.
Some investigations may need to be conducted to help with diagnosis and planning, such as CT scans, MRI scans, and biopsies. In cases where complex bony reconstruction is required, computer-aided planning and models may be used to ensure perfect reconstructive outcomes.
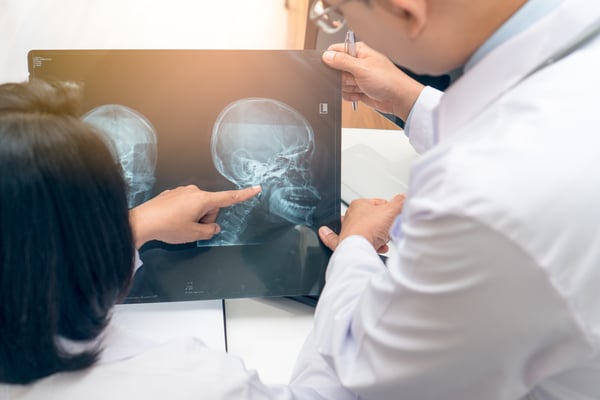
Post-operative care and recovery
Potential risks and complications
Further on in recovery, the focus will be on functional and aesthetic rehabilitation including minimizing the impact of scars and any radiotherapy effects, if the adjuvant therapy is performed. Any adjuvant radio- or chemotherapy needed can be commenced at the one-month post-operative mark once healing is shown to be going well.
Why choose Polaris Plastic Surgery?
Schedule a consultation with one of our doctors to assess your needs and goals. Through a thorough discussion, the appropriate reconstructive procedure to achieve the desired functional and aesthetic outcomes can be chosen.
FAQ
What is Computer-Aided Design (CAD) in head and neck reconstruction?
CAD in head and neck reconstruction involves the use of pre-operative scans, computer programs and 3D printers to create surgical aids and implants that aim to give the patient as close to a perfect reconstruction as possible. It is most used for head and neck defects requiring bony reconstruction. By bringing the surgical planning to the computer, this effectively increases the accuracy of tissue and bony shaping to the millimetre and cuts down operative time due to the printing of precise cutting guides, templates, and implants. An additional benefit is the ability for immediate dental restoration in select cases. Our plastic surgeon works closely with local and international teams in creating these surgical aids and will discuss their use and necessity with you.
What is minimally invasive and/or robotic-assisted head and neck reconstruction?
Minimally invasive head and neck reconstruction entails the use of small, well camouflaged incisions, commonly intra-orally, along with adjuncts such as the endoscope or surgical robots, to reconstruct hard-to-reach areas of the head and neck whilst minimizing scarring and surgical morbidity. This is performed for select cases where the avoidance of visible cuts in the face or through the facial skeleton is desirable, for example in cases where there has been previous radiotherapy. Dr Adrian is one of the only plastic surgeons in Singapore trained in the use of the surgical robot and will discuss whether this is a feasible option for your reconstruction.
Can radiation injury to the head and neck be treated?
Radiotherapy (RT) is an important adjunctive treatment in many cancers. In the head and neck, RT can be performed before or after surgery, depending on the cancer characteristics. Whilst RT can help eradicate microscopic cancer cells, it can also have a deleterious effect on normal tissue by inducing scarring and fibrosis. This can lead to debilitating symptoms such as neck tightness and pain, and the inability to fully open the jaw (trismus). Using treatments including botulinum toxin and fat transfer, our plastic surgeon can help to mitigate some of the effects of unwanted radiation injury, which can otherwise be a huge barrier to daily function.
Does head and neck reconstruction interfere with cancer surveillance?
In short, head and neck reconstruction does not interfere with cancer surveillance, even in hard-to-see regions. Besides visualization of the suspect area, there are other methods to detect cancer recurrence including clinical palpation and scans such as CT or PET scans.
Can I delay my head and neck reconstruction?
Head and neck defects often expose vital structures such as vessels, nerves, tendon, and bone. Oftentimes, they also expose the neck structures to salivary leak and potential infection and can be very aesthetically disfiguring. Whilst some head and neck reconstructive procedures can be delayed, it is seldom that the defects can stay prepped for reconstructive beyond the first 24 to 48 hours before definite reconstruction is required.
I previously had head and neck reconstructive procedures but am dissatisfied with some of the outcomes. Can I have reconstruction again?
Yes, you can. Most times, it is not possible to completely restore normality in one surgery. You can have secondary reconstructive procedures months or even years after the first procedure. Your surgeon will assess you and work with you to achieve your expectations using the best available methods. These may involve fat grafting, prosthesis, and/or flap procedures.
2. Ooi A SH, Teven CM, Inbal A, Chang DW. The Utility Of The Musculocutaneous Anterolateral Thigh Flap In Pharyngolaryngeal Reconstruction In The High-Risk Patient. J Surg Oncol 2017;115;842-47
3. Ooi A SH, Butz D, Gooi Z, Chang D W. Modification of the radial forearm fasciocutaneous flap in partial pharyngolaryngeal reconstruction to minimize fistula formation. Plast Reconstr Surg 2016;138:903-907
5. Ooi A, Feng J, Tan HK, Ong YS. Primary treatment of mandibular ameloblastoma with segmental resection and free fibula reconstruction: Achieving satisfactory outcomes with low implant-prosthetic rehabilitation uptake. J Plast Reconstr Aesthetic Surg. 2014;67:498-505
6. Ng MJM, Goh CSL, Ooi A SH. A Head-to-Head Comparison of the Medial Sural Artery Perforator versus Radial Forearm Flap for Tongue Reconstruction. J Reconstr Microsurg. 2020 Oct (doi: 10.1055/s-0040-1718551)
PATIENT STORIES
Post Massive Weight Loss Body Contouring
A 40-year-old lady consulted with Dr Pek with the desire to correct large amounts of excess skin and soft tissue. She had undergone Bariatric Surgery (Sleeve Gastrectomy) 2 years prior to her presentation and had successfully lost almost 30kg of weight. With ... Read more
Treat Gynecomastia with Minimally Invasive Methods in Singapore
A 38-year-old male engineer presented to Dr Pek with symptomatic growth of his chest/breast area. Since puberty, he complained of unusually prominent chest tissue around his nipple and areolar region. This had worsened gradually over the years, with the left ... Read more
Upper eyelid lift and eyebags rejuvenation
63 years old Chinese female with hypertension and hyperlipidemia presented to Dr Pek with significant droopiness of her upper eyelids on both sides, affecting the upper portion of her visual field. She would constantly feel that her upper eyelids were heavy, ... Read more
Bilateral breast reconstruction using abdominal free flaps
A 45-year-old mother of 2 children was diagnosed with left breast cancer, for which a skin-sparing mastectomy (total removal of breast tissue leaving behind the skin envelope) was recommended. Read more
ARTICLES
TL;DR: Breast implants can rupture over time, with signs ...
TL;DR Section: Your age shapes how breast augmentation ...
TL;DR: If diet and exercise haven’t fully shaped your ...
TL;DR: A tummy tuck (abdominoplasty) goes beyond aesthetics ...
Contact Form
1 Orchard Boulevard #10-08 Camden Medical Centre, Singapore 248649
6 Napier Rd, #08-01 Gleneagles Medical Center, Singapore 258499
Tel: +65 6737 4565 | Mobile: +65 8828 4565 | Email: clinic@polarisplasticsurgery.com | Business Hours: Mon - Fri: 9am - 6pm | Sat: 9am - 1pm | Sun/Ph: Closed











