Articles
How To Treat Lymphedema Without Surgery - Lymphedema Therapy
Lymphedema is the abnormal accumulation of fluid due to dysfunction in the lymphatic system. If you are at risk of lymphedema resulting from cancer treatment involving the removal of regional lymph nodes, lymphedema therapy can help reduce the risks. In this article, you will learn about the management techniques in lymphedema therapy and when surgery would be required. But first, let’s learn more about this condition, its causes and symptoms.
What is lymphedema?
Lymphedema occurs when the lymph system cannot remove fluid, fat, and proteins, causing limbs to swell and eventually become heavy, hard, painful, and inflexible. It also causes the limb to be more prone to infections, as the lymph system helps with the immune system of the body.
Traditionally, patients can manage lymphedema conservatively with lymphedema therapy. Lymphedema therapy can include physical therapy that helps to relieve swelling by moving lymphatic fluid out of the affected area. This includes manual decongestive therapy, lymphatic massage, use of pressure garments, or serial wrapping of the affected limb to encourage fluid egress back to the circulation.
Signs & Symptoms, and What Causes Lymphedema (in Legs)
Lymphedema is characterised by a progressive and often persistent swelling of a limb, particularly the arms or legs, and recognising the key lymphedema symptoms early can dramatically improve outcomes. Commonly, the affected leg begins to feel heavier than usual or tight — you may notice that rings, shoes, or socks feel snugger by evening. The skin may appear stretched or shiny and may sometimes feel warmer than its counterpart. As fluid builds up, you may experience reduced mobility, a feeling of fullness, and discomfort or aching. Over time, the tissue can become firm or fibrotic (hardened) and the skin may show changes such as crepiness or thickening, signalling a more advanced stage of lymphedema.
Turning to what causes lymphedema in legs, the underlying trigger is a disrupted lymphatic drainage system that fails to efficiently remove interstitial fluid, fat and proteins. In the leg region this can happen after surgical removal of lymph nodes (for example in cancer treatment), radiation therapy, traumatic injury or infection that damages lymph vessels. In some cases, the cause is congenital or developmental — known as primary lymphedema — where the lymphatic system is malformed from birth, though this tends to present later in life. Additional risk factors specific to legs include chronic venous insufficiency, obesity, immobility, or repeated episodes of cellulitis that continuously impair lymph transport. These factors contribute to fluid pooling, tissue changes and increased susceptibility to skin breakdown or infection.
Recognising both the symptoms and the causes early allows timely intervention with therapies (manual drainage, compression, skin care and exercise) to lessen progression and reduce complications.
Lifestyle changes to help with managing lymphedema
Making lifestyle changes to support the outcome of your lymphedema therapy is important in maintaining good results. Here are some areas in which you may need to make some adjustments:
Food
Your diet plays an important role in managing lymphedema and reducing the risk of complications. Opt for low fat and nutrient-dense foods such as lean proteins, whole grains, fruits, vegetables, and green leaves in your daily nutrition. This can help you load up on vitamins and minerals, fight infections, and consume healthy proteins for overall nutrition.

Avoid high salt foods as sodium promotes fluid retention and aggravates lymphedema. Studies have shown that weight loss can improve lymphedema symptoms. To maintain a healthy weight, avoid foods high in sugar, saturated fats and trans fats. You may consume monounsaturated and polyunsaturated fats, which are considered ‘healthy fats’. They are found in foods such as olives, canola, avocado, sesame, and pumpkin.
If you have diabetes, managing your blood sugar levels is crucial in avoiding complications like infections and cellulitis. Try to eat foods with a low glycaemic index (GI) of 55 or less, such as low-fat dairy foods and nuts. The glycaemic index is a ranking of carbohydrates in foods. Foods with a low GI index can be digested gradually, resulting in a slow rise in blood glucose.
Minimize consumption of refined sugar and refined grains as these have been stripped of fibre and nutrients. A healthier alternative would be brown sugar, which allows gradual release of glucose into the bloodstream.
Additionally, alcohol consumption can cause blood vessels to expand, leading to increased swelling of the affected limb. Minimize consuming alcohol or food containing any amount of alcohol for effective lymphedema management.
Physical activity

Image: Lisa Schulz / Shutterstock.com
Studies have shown that exercise can reduce lymphedema flare-ups by restoring strength and flexibility, reducing weight, and improving drainage. Working with a lymphedema therapist who can customize a treatment plan that meets your needs and current fitness level is recommended.
Typically, an exercise plan for lymphedema patients includes a combination of strength training, flexibility and stretching exercises, and aerobic exercises that help in weight loss and promote deep breathing.
Massage
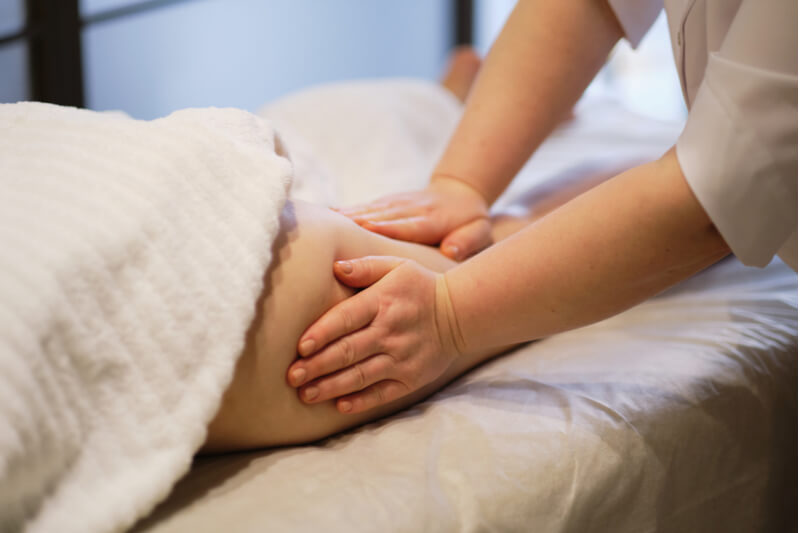
Lymphatic massage is also known as lymphatic draining or manual lymph drainage. Consult your doctor to request a referral to a therapist skilled in lymphatic massage. This involves massaging the skin in directions following the lymphatic system’s structure so that accumulated lymph fluid can drain through the right channels.
The massage is usually gentle with no pain involved. Your therapist may also teach self-massage exercises designed to encourage the flow of lymphatic fluid out of the affected limb.
Skin Care
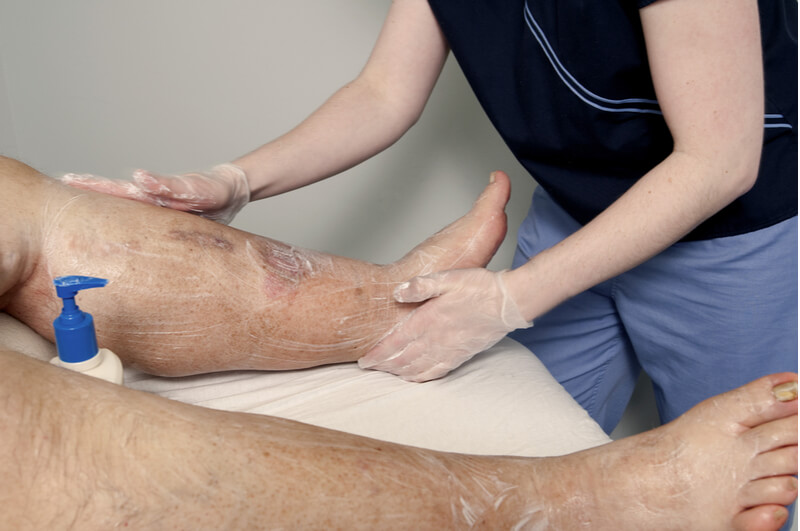
Skin care is an important part of conservative lymphedema therapy. This includes daily moisturizing of the skin to keep it soft and supple, avoiding dryness and cracking which may lead to itching and act as entry points for infection.
It is also important to avoid any sort of injury to the skin of the affected limb, including insect bites and small cuts. If these do happen, keep the wound meticulously clean and consult your doctor, who may prescribe you a course of antibiotics to reduce the risk of infection to the lymphedematous limb.
Compression Garments/Wrapping

Fluid accumulation in the lymphedematous limb can be managed by compression garments or wrapping.
Wrapping the affected limb(s) in layered bandages is an effective method that can be done on your own to manage any increased accumulation of fluid in between your doctor consultations. However, it is important to consult your lymphedema therapist, who can teach you the correct procedure and techniques. The layers also help protect the skin from irritation, spread compression evenly across affected areas, and encourage lymph flow.
Tailored compression garments are used for maintenance and can be worn all day, exerting low pressure when your muscles are at rest, and avoiding constriction lymph blockage when you sleep.
What is the cost of lymphedema therapy?

A single session of manual lymph drainage may cost between $250 to $400 in Singapore, depending on the specialist, treatment plan, and number of limbs affected. However, since lymphedema therapy requires major lifestyle changes and long-term therapy sessions, it is best to consult an experienced and skilled specialist who can provide comprehensive management. A plastic surgeon specializing in lymphedema treatment can help with coordinating your overall management.
Consider lymphedema surgery for more severe cases
Most doctors will recommend lymphedema therapy only for the early stages of lymphedema. Once lymphedema has progressed to irreversible swelling or skin changes, surgery is recommended to restore lymphatic flow. Surgical options include physiological and excisional procedures.
Physiological procedures involve rewiring the lymphatic system within the affected limb, while excisional methods remove diseased tissue. If there is no improvement after thorough use of conservative treatment, then lymphedema surgery will be needed.
Why surgery may be recommended

Conservative management is more of a temporary fix and does not solve the underlying disruption in lymphatic flow. In the past decade, surgical treatments for lymphedema have improved significantly. Most of the developments have been in physiological treatments aimed at restoring the dysfunctional lymphatic system.
This includes lymphaticovenous bypass/anastomosis (LVB/LVA) surgery and vascularized lymph node transfer (VLNT).
In LVB, special machines and techniques identify the clogged lymphatics and divert their flow by suturing them to neighbouring veins. This procedure is extremely low risk, can be performed under local anaesthesia, and requires very small incisions and minimal downtime.
For VLNT, lymph nodes are taken from a part of your body where lymph nodes are in excess and transplanted to the affected limb. VLNT usually requires a few days of hospital stay and about 1 to 2 weeks of downtime.
In severe cases of lymphedema involving permanent, disfiguring skin changes, physiological techniques may no longer be possible. For these situations, excisional surgery such as liposuction or removal of fibrotic skin can be performed to debulk the affected body part.
Post-surgery, patients will still have to continue taking care of their lymphedema. However, many patients report reduced symptoms, and some even completely stop lymphedema therapy altogether.
Managing Lymphedema
Lymphedema is a condition that can be managed well with the right care and expertise. Speak to our board-certified plastic surgeon Dr Adrian Ooi, who is experienced in lymphedema treatment.
FAQs about lymphedema surgery
- What happens during surgery?
You will be admitted to the hospital the day before or on the day of surgery. If a general anaesthetic (GA) is planned, you will need to fast for at least 8 hours before surgery. LVBs can often be performed under local anaesthesia with or without sedation or GA in a day surgery setting. If a VLNT or excisional techniques are planned, you may require a few days’ hospital stays. In general, lymphedema surgery can last from 3 to 6 hours.
- What are the risks and complications of surgery?
General risks include pain, bleeding, and infection. However, post-surgery pain is well controlled with medication, with a low risk of bleeding and infection. Specific to VLNT, if there are any issues with the blood supply to the transferred lymph nodes, you may be brought back to the operating theatre. There may be some scarring and numbness in the affected area, but the doctor will usually provide instructions to manage this well.
Contact Form
1 Orchard Boulevard #10-08 Camden Medical Centre, Singapore 248649
6 Napier Rd, #08-01 Gleneagles Medical Center, Singapore 258499
Tel: +65 6737 4565 | Mobile: +65 8828 4565 | Email: clinic@polarisplasticsurgery.com | Business Hours: Mon - Fri: 9am - 6pm | Sat: 9am - 1pm | Sun/Ph: Closed











